Confronting Complexity: Chronic Diseases Amidst Cancer Diagnosis
- gilliangillies0
- Mar 4, 2024
- 4 min read
Updated: Apr 1, 2024

In cancer care, the presence of pre-existing chronic diseases among individuals with suspected cancer symptoms can significantly impact diagnostic efficiency and the stage of cancer at diagnosis (Renzi, 2019). Shared risk factors such as smoking and obesity contribute to the common occurrence of chronic conditions among cancer patients (Jiang, 2021). Notably, certain cancer types, including ovarian cancer, chronic leukemias, some lymphomas, and metastatic breast or prostate cancer, can manifest as chronic illnesses akin to diabetes or heart disease (American Cancer Society, 2019).
In my practice within cancer care, it's routine to encounter patients dealing not only with cancer but also with various chronic conditions. Surprisingly, research indicates that approximately 75% of individuals diagnosed with cancer have at least one other chronic health condition (Kone, 2021). Managing multiple chronic diseases not only escalates the complexity of care but also heightens the risk of adverse outcomes (Mahamud, 2020).
In 2021, Eastern Canada was projected to have high cancer incidence rates (Canadian Cancer Society, 2021). Specifically, in my province of New Brunswick, there were around 5,500 new cases expected in 2023 (Canadian Cancer Society, 2023).
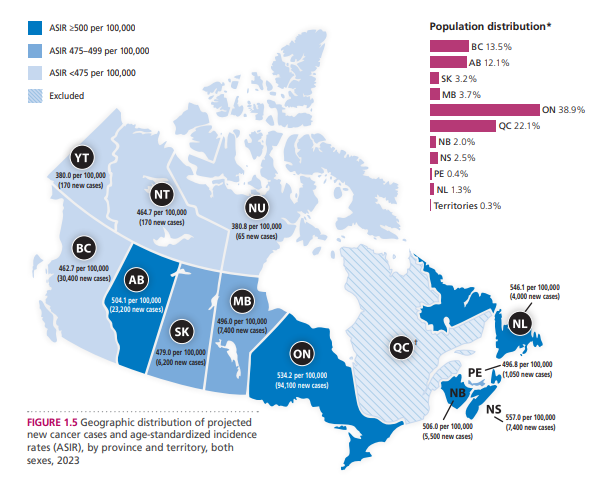
(Canadian Cancer Society, 2023)
There are many interconnecting chronic conditions that coexist within cancer care. Some common chronic diseases frequently identified in oncology patients include:
Hypertension
Chronic obstructive pulmonary disease (COPD)
Diabetes
Cardiovascular Disease (CVD)
Congestive Heart Failure (CHF) (Kone, 2021).
What are the rates of Chronic disease rates studied in Cancer Care?
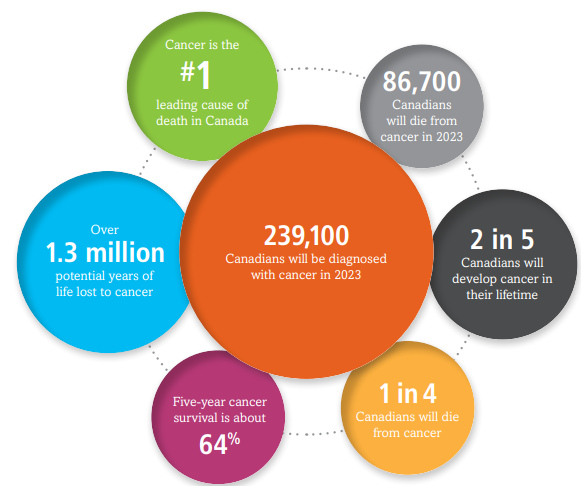
Rates of chronic diseases I encounter in cancer care is unfortunately high. In one study from Ontario, more than 75% of people with cancer have at least one type prevalent chronic conditions. The chronic conditions can vary by cancer type and can have different impacts on patient outcomes (Kone, 2021). Unfortunately, the number of chronic conditions continues to increase substantially after a cancer diagnosis, and it can be challenging to manage (Mahmud, 2020, Phillips, 2010). On a global level, Australia reported 61% of patients experienced one chronic disease condition with a cancer diagnosis, and 21% with 3 or more chronic conditions (Mahmud, 2020), where Jiang (2020) did a study in the United States capturing 72% of cancer survivors with multiple chronic conditions. The below figure captures 26.4% of Canadians were expected to be diagnosed and die with cancer last year (Canadian Cancer Society, 2023). This compares to other chronic disease.

(Canadian Cancer Society, 2023)
Primary Determinants
In cancer practices, particularly when dealing with populations, several primary determinants of chronic diseases are commonly encountered. These determinants play a crucial role in shaping cancer incidence, progression, treatment outcomes, and overall population health. Some of the primary determinants include:
Lifestyle Choices: Unhealthy lifestyle habits such as smoking, excessive alcohol consumption, poor diet, lack of physical activity, and obesity are well-established risk factors for various types of cancer (Jiang, 2021; Mahmud, 2020).
Socioeconomic Factors: Socioeconomic factors such as sex, income, education, occupation, marital status, and access to healthcare services significantly influence cancer prevention, diagnosis, and treatment outcomes (Mahmud, 2020).
Access to Healthcare: Limited access to healthcare services, including screenings, early detection programs, and diagnostic tools, can impede timely cancer diagnosis and treatment initiation (Mahmud, 2020). For instance, only 34% of New Brunswickers reported being able to access their Primary Care provider within 5 business days, reflecting potential barriers to timely healthcare access (NBHC, 2022).
So how do we handle chronic diseases in the Oncology Setting? This question is very interesting. Managing chronic diseases in the oncology setting poses significant clinical challenges, particularly as many cancer patients also suffer from comorbid conditions (Mahmud, 2020). Early diagnosis remains paramount in improving cancer outcomes (Renzi, 2019). However, the predominant approach in care plans often prioritizes cancer treatment over managing concurrent chronic conditions, despite evidence suggesting that coordinated management could enhance patient outcomes (Kone, 2021).
To address this disparity, implementing coordinated care pathways is essential to reduce treatment burden and optimize patient care (Kone, 2021). Integrating rehabilitation or individualized survivorship approaches can help alleviate patient challenges and promote long-term maintenance (Phillips, 2010). In consultation with some oncologists where I work at the Dr. Everett Chalmers Hospital, many follow the American Society of Clinical Oncology (ASCO) guidelines. These guidelines highlight the importance of managing comorbid conditions amidst the rapidly growing cancer survivor population (Jiang, 2021; Shapiro, 2016).
Utilizing a multidisciplinary team approach, with primary care physicians playing a prominent role, has shown promise in managing chronic care effectively (Phillips, 2010). By leveraging the expertise of various healthcare professionals, including oncologists, primary care providers, and rehabilitation specialists, comprehensive care can be tailored to meet the unique needs of cancer patients with chronic conditions.
References:
American Cancer Society (2019, January 14). Managing Cancer as Chronic Disease Illness. Retrieved March 2, 2024, from https://www.cancer.org/cancer/survivorship/long-term-health-concerns/cancer-as-a-chronic-illness.html
Canadian Cancer Society (2023, November 1). Canadian Cancer Statistics. Retrieved March 4, 2024, from https://cdn.cancer.ca/-/media/files/research/cancer-statistics/2023-statistics/2023_pdf_en.pdf?rev=7e0c86ef787d425081008ed22377754d&hash=DBD6818195657364D831AF0641C4B45C&_gl=1*e86npi*_gcl_au*NjQyMTU0NTE3LjE3MDU3NjUxNjI
Canadian Cancer Society (2021, November 1). Canadian Cancer Statistics. Retrieved March 4, 2024, from. https://cdn.cancer.ca/-/media/files/research/cancer-statistics/2021-statistics/2021-pdf-en-final.pdf
Jiang, C., Deng, L., Karr, M. A., Wen, Y., Wang, Q., Perimbeti, S., Shapiro, C. L., & Han, X. (2021). Chronic comorbid conditions among adult cancer survivors in the United States: Results from the National Health Interview Survey, 2002‐2018. Cancer. https://doi.org/10.1002/cncr.33981
Koné, A. P., & Scharf, D. (2021). Prevalence of multimorbidity in adults with cancer, and associated health service utilization in Ontario, Canada: a population-based retrospective cohort study. BMC Cancer, 21(1). https://doi.org/10.1186/s12885-021-08102-1
Mahumud, R. A., Alam, K., Dunn, J., & Gow, J. (2020). The burden of chronic diseases among Australian cancer patients: Evidence from a longitudinal exploration, 2007-2017. PLOS ONE, 15(2), e0228744. https://doi.org/10.1371/journal.pone.0228744
New Brunswick Health Council (2022). Primary Care Survey. Retrieved February 16, 2024, from Needs of New Brunswickers. (2022). Nbhc.ca. https://nbhc.ca/table/needs-new-brunswickers?cuts=NB%2CNBZ1%2CNBZ2%2CNBZ3%2CNBZ4%2CNBZ5%2CNBZ6%2CNBZ7&gid=8207&sid=5284&tid=5284
Phillips, J. L., & Currow, D. C. (2010). Cancer as a chronic disease. Collegian, 17(2), 47–50. https://doi.org/10.1016/j.colegn.2010.04.007
Renzi, C., Kaushal, A., Emery, J. (2019). Comorbid chronic diseases and cancer diagnosis: disease-specific effects and underlying mechanisms. Nat Rev Clin Oncol 16, 746–761. https://doi.org/10.1038/s41571-019-0249-6
Shapiro, C. L., Jacobsen, P. B., Henderson, T., Hurria, A., Nekhlyudov, L., Ng, A., Surbone, A., Mayer, D. K., & Rowland, J. H. (2017). ReCAP: ASCO Core Curriculum for Cancer Survivorship Education. JOP, 12(2), 145. https://doi.org/10.1200/JOP.2015.009449


Comments